
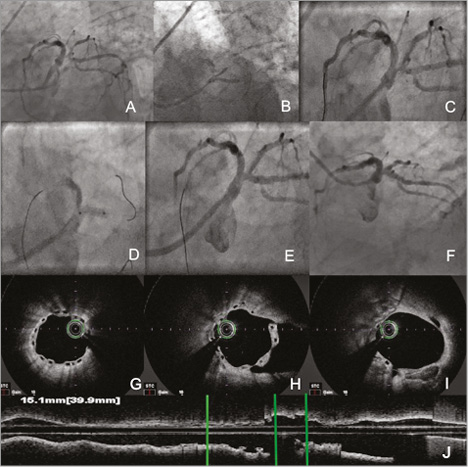
A 72-year-old man with class III angina and positive stress test underwent coronary angiography which showed subocclusive stenosis of the distal left main coronary artery (LMCA) trifurcation, involving the ramus intermedius and the left circumflex artery (LCx) ostium (Panel A, Moving image 1). The patient underwent trifurcation reconstruction through kissing balloon inflation with two second-generation drug-coated balloons (DCB) (Elutax SV; Aachen Resonance, Aachen, Germany) in the two involved branches and subsequent bioresorbable vascular scaffold (3.0×12 mm Absorb BVS; Abbott Vascular, Santa Clara, CA, USA) implantation beginning from the LCx ostium because of a non-optimal angiographic result after DCB use (Panel B, Panel C, Moving image 2). The final result showed complete reconstruction of the distal LMCA (Panel D, Panel E, Moving image 3). One-year angiographic follow-up confirmed the persisting good result, with optical coherence tomography showing an optimal BVS apposition to the vessel wall with complete coverage of all visible struts (Panel F-Panel J, Moving image 4, Moving image 5).
Currently available devices allow the treatment of complex lesions such as a distal LMCA with trifurcation. The use of metallic stents might result, as in this case, in left anterior descending artery impairment or in a subsequent increased risk of restenosis or stent thrombosis. Thanks to their limited persistence in the vessel, the combined use of DCB and bail-out BVS, two relatively new devices which are gradually expanding their indications for use, have the ambitious aim of treating/reconstructing complex coronary lesions at sites where the use of common stents might be a risky strategy in the long term, finally returning the vessel wall to its original state.
Conflict of interest statement
The authors have no conflicts of interest to declare.
Supplementary data
Moving image 1. Basal angiography.
Moving image 2. Angiography after DCB-PCI, type C dissection in proximal left circumflex artery.
Moving image 3. Final angiography after BVS implantation.
Moving image 4. One-year angiographic follow-up.
Moving image 5. One-year OCT follow-up.
Supplementary data
To read the full content of this article, please download the PDF.
Basal angiography.
Angiography after DCB-PCI, type C dissection in proximal left circumflex artery.
Final angiography after BVS implantation.
One-year angiographic follow-up.
One-year OCT follow-up.

