Abstract
BACKGROUND: Percutaneous suture-based arterial access site closure (ProGlide) is commonly applied in patients undergoing transfemoral transcatheter aortic valve implantation (TAVI). However, the failure of a suture-based vascular closure device (VCD) may require additional treatment.
AIMS: We aimed to evaluate the efficacy and safety of bailout access site closure using a large-bore plug-based device (MANTA) in patients with failed suture-based closure during transfemoral TAVI.
METHODS: Patients undergoing a bailout attempt with the MANTA VCD were identified from a prospectively enrolling, institutional registry. Efficacy was defined as haemostasis at the access site without the need for alternative treatment other than manual compression or endovascular ballooning. Safety was defined as freedom from vascular dissection, stenosis and occlusion requiring intervention.
RESULTS: Of 2,505 patients, 66 underwent a bailout attempt with MANTA as a result of ProGlide failure, which occurred before the large-bore sheath insertion in 16.7% of patients and after the sheath removal in 83.3% of patients. Bailout MANTA was deemed effective in 75.8% of patients (50/66), and the technique was considered safe in 86.4% (57/66) of patients. Failure of bailout MANTA occurred because of its superficial application, resulting in persistent bleeding in 18.2% of patients (12/66), and because of its deep application, resulting in stenosis or occlusion in 6.1% of patients (4/66). Operator experience with the technique (odds ratio [OR] 12.29, 95% confidence interval [CI]: 1.99-75.99; p=0.007) and prior use of three ProGlides (OR 0.02, 95% CI: <0.01-0.39; p=0.010) were the only independent predictors of the efficacy endpoint.
CONCLUSIONS: Bailout MANTA after ProGlide failure was effective and safe, but operator experience seems to be crucial. Further technological refinements to facilitate accurate placement appear necessary.
Vascular closure is a critical element of any transfemoral transcatheter aortic valve implantation (TAVI), and the percutaneous suture-based closure technique using the Perclose ProGlide device (Abbott) is the most widely applied in clinical practice12. However, despite a decade of experience, suture-based vascular closure device (VCD) failure occurs in 5.4% to 8.0% of procedures and is associated with prolonged hospitalisation34. In case of VCD failure, the interventionalist has few options for vascular access site closure. As a first step, additional suture-based VCDs can be applied. Supportive options may include prolonged manual compression and endovascular ballooning. Stenting is commonly required to avoid surgical repair if haemostasis cannot be achieved with the previously mentioned interventions.
The MANTA (Teleflex) VCD is a new-generation device specifically designed for large-bore vascular closure, relying on a plug-based rather than a suture-based mechanism. In the randomised MASH trial, no differences were observed between the MANTA and the suture-based ProGlide VCD in terms of vascular complications or bleeding events5. However, in the larger randomised CHOICE-CLOSURE trial, access site-related vascular complications occurred more frequently with the MANTA VCD6.
Anecdotally, the MANTA device has been used as a bailout VCD if vascular closure could not be achieved with suture-based VCDs56, which could reduce the need for unplanned endovascular or surgical interventions. However, the safety and success rates of this technique have not been systematically analysed. Therefore, we sought to investigate the efficacy and safety of the bailout MANTA technique after suture-based VCD failure in a large, consecutive, well-defined cohort of patients undergoing transfemoral TAVI.
Methods
PATIENT POPULATION
All patients undergoing bailout arterial access site closure with MANTA during transfemoral TAVI between the introduction of the device in September 2019 and November 2022 were identified from the institutional database of the Heart Center Leipzig at the University of Leipzig. Patient demographics, clinical and procedural data were prospectively collected as part of a dedicated institutional registry (ClinicalTrials.gov: NCT05015452) approved by the local ethics committee. All patients provided written informed consent. A reference cohort of patients with elective vascular closure with MANTA from the randomised CHOICE-CLOSURE trial was also included6.
PROCEDURAL DETAILS
All TAVI procedures and access site selection were planned with contrast-enhanced multislice computed tomography. Vascular access site calcification was classified as none, mild, moderate, or severe, according to the previously published MASH classification5. The decision to perform TAVI and access site selection were made by a multidisciplinary Heart Team.
Pre-existing antiplatelet therapy was not changed before TAVI. Direct oral anticoagulants were discontinued 24-36 hours before the procedure, depending on renal function. Vitamin K antagonists were maintained, aiming for an international normalised ratio (INR) between 2.0 and 2.5 on the day of the procedure.
Puncture of the main access site was performed using the previously described roadmapping technique8 or with ultrasound guidance. The choice of puncture technique was made by the operator. Patients received intravenous unfractionated heparin during the procedure, and the target activated clotting time (ACT) was set at 250-300 seconds. At the end of the TAVI procedure, a reduced dose of protamine (500 IU/1000 IU heparin) was regularly administered to reduce the ACT to less than 250 seconds, followed by application of the VCD. The use of the full dose of protamine (1000 IU/1000 IU of heparin) was left to the operator’s discretion.
A peripheral angiogram was subsequently performed to assess vascular closure, bleeding, and vascular complications.
DEVICE CHARACTERISTICS
The ProGlide VCD was the only suture-based VCD used at the Heart Center Leipzig during the study period. Above 8 French (Fr), the use of two ProGlide VCDs is recommended, but several studies have shown that one ProGlide VCD can also be sufficient for safe vascular closure910. The device is based on a suture-mediated closure principle. A detailed description regarding the application of the ProGlide VCD has already been provided elsewhere11. A crucial aspect of the device is the fact that wire access is maintained even after the sheath is removed and the sutures are tightened. Therefore, the ProGlide VCD offers the possibility of subsequently applying a different VCD if necessary.
The plug-based MANTA VCD consists of three parts: a luminal resorbable polymer toggle, an extraluminal collagen plug attached to a non-resorbable polyester suture, and a stainless-steel lock. The system is available in two sizes: 14 Fr and 18 Fr. Both sizes were used in this study. In an elective MANTA VCD setting, an 8 Fr depth locator is used to determine the implantation depth prior to the insertion of the large sheath. Further technical details of the device and its application have been described elsewhere12. Once the MANTA VCD is deployed, there is no guidewire left in the vessel and no more VCDs can be applied.
MANTA BAILOUT TECHNIQUE
Suture-based VCD failure can either occur as an upstream event prior to the insertion of the large-bore sheath, or as a downstream event after sheath removal. The preimplant depth measurement of a MANTA VCD in a downstream bailout situation can be more challenging than in an elective procedure due to two factors. First, the vascular puncture site after large-bore sheath removal is significantly larger than before its insertion, which leads to permanent bleeding next to the 8 Fr MANTA implantation depth locator. Consequently, measurement of the puncture depth could be inaccurate. Second, the groin tissue may significantly swell during the procedure, further impacting measurement accuracy.
We have gradually introduced a few modifications to the MANTA VCD measurement and application technique in order to address these difficulties. First, measurement of the implantation depth is performed under slight compression of the surrounding tissue. Bleeding through the access site can thereby be reduced and accurate measurements obtained. Second, two centimetres are added to the measured puncture depth (instead of one centimetre in elective procedures). Finally, the success of the bailout MANTA procedure must be verified by angiography. In this study, operators defined as having “MANTA bailout experience” were those who had performed 10 or more bailout procedures.
VASCULAR CLOSURE AND VCD FAILURE STRATEGIES
During the study period, the bailout MANTA technique was implemented into the hospital’s internal workflow for vascular closure and complication management after TAVI (Figure 1). Preclosure was most commonly performed with one ProGlide, which could be followed by one to two additional ProGlides if VCD application was not successful or haemostasis was inadequate. If the suture-based VCD achieved a significant but incomplete reduction in bleeding from the access site, a final small plug-based VCD (Angio-Seal; Terumo) was used for completion of haemostasis. In this context, the Angio-Seal was not used as a bailout device but as part of the planned closure strategy1314. If the ProGlide VCD could not be inserted prior to the procedure or if there was no significant haemostasis with ProGlide after the procedure, a bailout MANTA was considered. The decision for bailout MANTA was left to the operator’s discretion. A second arterial access was routinely obtained to allow supportive crossover interventions in case of vascular complications or VCD failure. These included endovascular balloon inflation at the access site in case of bleeding or to treat stenosis or dissection. In addition, endovascular balloon inflation was sometimes accompanied by an injection of fibrin to treat access site bleeding15. However, implantation of a stent or vascular surgery could not always be avoided.
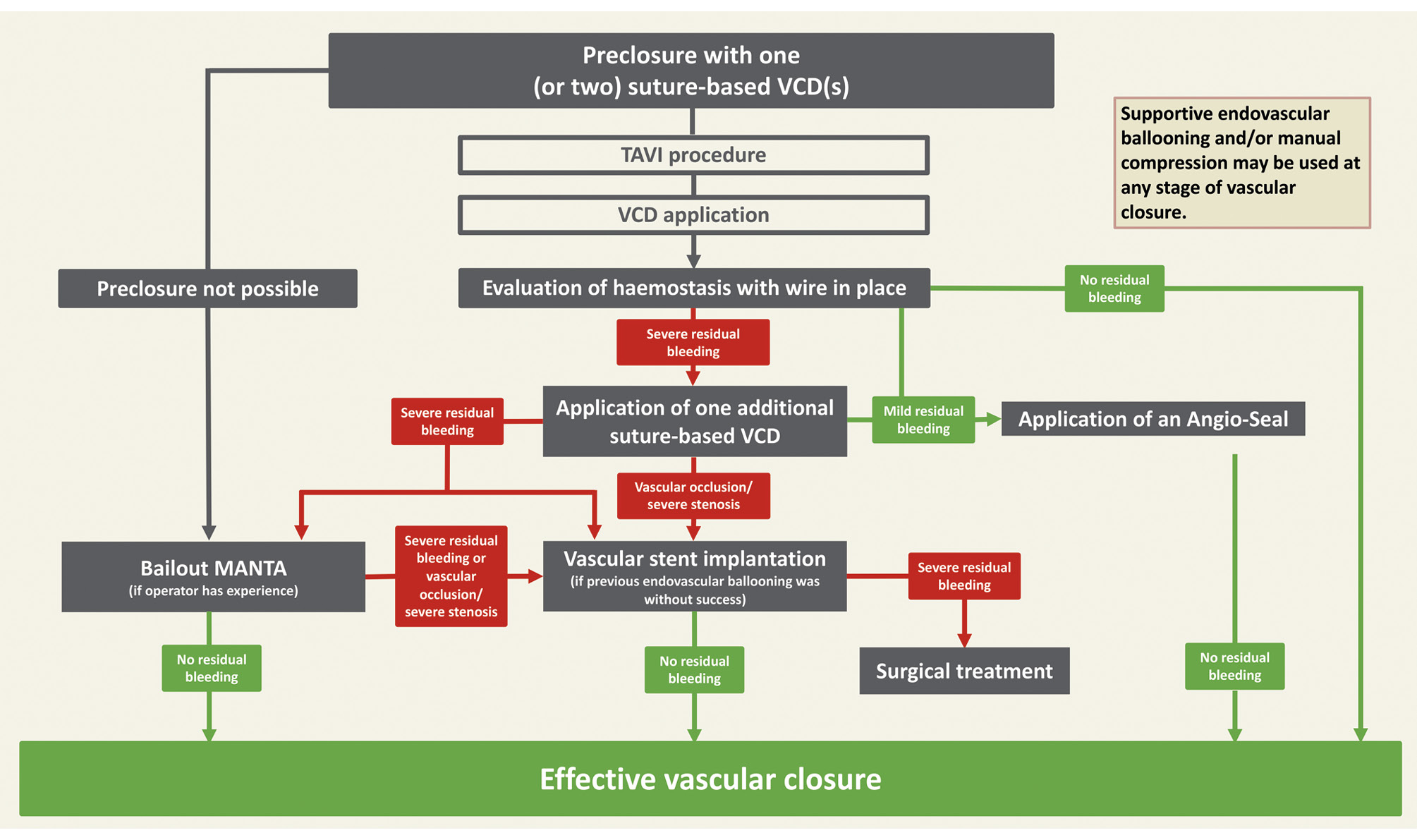
Figure 1. Vascular closure and bailout strategies after transfemoral transcatheter aortic valve implantation. TAVI: transcatheter aortic valve implantation; VCD: vascular closure device
STUDY ENDPOINTS
The primary objective of this study was to assess both the efficacy and safety of the bailout MANTA technique. Efficacy was defined as achieving haemostasis without the need for alternative interventions, except manual compression or endovascular ballooning. If the efficacy endpoint was not met, the MANTA bailout procedure was deemed to have failed. Safety was defined as freedom from vascular dissection, stenosis or occlusion requiring interventional or surgical treatment. These endpoints were assessed in both the study population and the reference elective MANTA cohort of the CHOICE-CLOSURE trial. In order to examine the presence or absence of a learning curve, efficacy and safety endpoints were assessed for each tertile of patient enrolment. In addition, potential predictors of the efficacy endpoint were analysed.
STATISTICAL ANALYSIS
Continuous data are presented as mean (±standard deviation) or median (interquartile range [IQR]), as appropriate, and categorical data as number and proportion (%). Data distribution was tested for normality using the Kolmogorov-Smirnov and Shapiro-Wilk tests. Differences between groups were tested with the Student’s t-test or Mann-Whitney U test (continuous data) and Chi-square test or Fisher’s exact test (categorical variables). Univariable and multivariable logistic regression analysis was performed to analyse potential predictors of the efficacy endpoint. Known risk factors and possible influencing variables for VCD failure were included in the univariable analysis. All variables with a p-value<0.05 were used for the multivariable analysis. A two-sided p-value of <0.05 was considered statistically significant. Statistical analysis was performed using SPSS Version 26.0 statistical software (IBM).
Results
BASELINE AND PROCEDURAL CHARACTERISTICS
Between September 2019 and November 2022, a total of 3,267 patients were treated with transfemoral TAVI. Of these, 2,505 patients received the suture-based ProGlide VCD as a primary vascular closure strategy. ProGlide VCD failure was observed in 4.3% (107/2,505) of these patients, of whom 61.7% (66/107) underwent a bailout MANTA attempt. The treatment of patients with suture-based VCD failure without a bailout MANTA attempt is detailed in Supplementary Table 1.
Most of the bailout MANTA patients were elderly (mean age 81.1±5.9 years) and had a low to intermediate Society of Thoracic Surgeons score (3.5 [2.3-6.4]) (Table 1). The mean body mass index (BMI) was 29.4±5.5 kg/m², peripheral vascular disease was present in 7.3% of patients, and the mean diameter of the common femoral artery access site was 7.6±1.6 mm (Supplementary Table 2). Overall, more than half of the patients had moderate (33.3%) or severe (31.8%) calcification of the iliofemoral access vessels. Furthermore, anterior calcification of the access site was prevalent in almost half of the study patients (45.5%).
Procedural details are provided in Supplementary Table 3. A total of 24.2% of access site punctures were performed under ultrasound guidance (all others by angiographic roadmap guidance).
Suture-based VCD failure occurred upstream (before large-bore sheath introduction) in 16.7% of patients and downstream (after sheath removal) in 83.3% of patients. Bailout MANTA was used after the failure of one ProGlide VCD in 30.3%, after the failure of two ProGlides in 60.6%, and following the failure of three ProGlides in 9.1% of patients. The 18 Fr MANTA VCD was used in the majority of bailout cases (74.2%).
Table 1. Baseline clinical characteristics.
| Variable | N=66 |
|---|---|
| Age, years | 81.1±5.9 |
| Female sex | 28 (42.6) |
| Body mass index, kg/m² | 29.4±5.5 |
| Logistic EuroSCORE I | 12.1 (6.5-18.0) |
| Society of Thoracic Surgeons score, % | 3.5 (2.3-6.4) |
| New York Heart Association Functional Class | |
| Class I | 5 (7.6) |
| Class II | 11 (16.7) |
| Class III | 44 (66.7) |
| Class IV | 6 (9.1) |
| Diabetes mellitus | 37 (56.1) |
| Coronary artery disease | 39 (59.1) |
| Previous myocardial infarction | 6 (9.1) |
| Previous CABG | 3 (4.5) |
| Previous PCI | 12 (18.2) |
| Previous valve surgery | 7 (10.6) |
| Cerebral vascular disease | 15 (22.7) |
| Previous stroke | 11 (16.7) |
| Peripheral vascular disease | 5 (7.6) |
| Previous peripheral intervention | 2 (3.0) |
| Atrial fibrillation | 29 (43.9) |
| Chronic dialysis | 2 (3.0) |
| Severe chronic renal failure* | 12 (18.2) |
| Baseline creatinine level, μmol/l | 108.0 (85.0-136.0) |
| Baseline haemoglobin level, mmol/l | 7.5±1.1 |
| Baseline INR | 1.1 (1.0-1.2) |
| Baseline platelet count, 109/l | 204 (161-265) |
| Baseline NT-proBNP level, ng/l | 2,369 (910-5,776) |
| Antiplatelets/anticoagulation | |
| None | 11 (16.7) |
| Single antiplatelet therapy | 26 (39.4) |
| Dual antiplatelet therapy | 0 (0) |
| Oral anticoagulation | 25 (37.9) |
| Oral anticoagulation and antiplatelet therapy | 4 (6.1) |
| Values are expressed as mean±SD or median (interquartile range) or n/N (%). *defined as a glomerular filtration rate <30 ml/min/1.73 m2 CABG: coronary artery bypass grafting; EuroSCORE: European System for Cardiac Operative Risk Evaluation; INR: international normalised ratio; N: number; NT-proBNP: N-terminal pro-brain natriuretic peptide; PCI: percutaneous coronary intervention; SD: standard deviation | |
EFFICACY AND SAFETY OF BAILOUT MANTA
In 54 (81.8%) patients, haemostasis was achieved with the MANTA bailout technique (Table 2). Among this group, seven patients required additional endovascular ballooning and four patients required prolonged manual compression to achieve complete haemostasis. After haemostasis, four patients needed vascular surgery or stenting due to vascular complications (vascular stenosis or occlusion). Thus, the efficacy endpoint was met in 50 patients (75.8%) (Central illustration). The number of successful MANTA bailouts increased numerically after the first tertile of patient recruitment. However, there was no statistically significant learning curve on the institutional level throughout the temporal tertiles of patient enrolment (Figure 2).
Haemostasis could not be achieved with the bailout MANTA technique in 12 patients (19.7%). Stent implantation was required in 9 of these patients, and 3 patients were treated with injection of thrombin during endovascular ballooning.
The safety endpoint was met in 57 patients (86.4%) (Table 2). The most frequent vascular complication was vascular stenosis (n=6), which was treated with endovascular ballooning and/or stenting in all patients. Two patients had complete vascular occlusions after bailout MANTA application, which required stenting in one case and surgery in the other. One patient had a vascular dissection that was managed by endovascular ballooning.
Overall, 12 patients (19.7%) needed vascular stenting despite bailout MANTA due to persistent bleeding (n=9) or vascular stenosis or occlusion (n=3).
Table 2. Main study outcomes.
| Variable | N=66 |
|---|---|
| Efficacy of bailout MANTA | 50 (75.8) |
| Haemostasis after bailout MANTA | 54 (81.8) |
| Haemostasis without additional support | 43 (65.2) |
| Haemostasis after additional manual compression | 4 (6.1) |
| Haemostasis after additional endovascular ballooning | 7 (10.6) |
| No haemostasis after bailout MANTA | 12 (18.2) |
| Need for stent implantation for haemostasis | 9 (13.6) |
| Pseudoaneurysm with need for thrombin injection | 3 (4.5) |
| Safety of bailout MANTA | 57 (86.4) |
| Complete vascular occlusion | 2 (3.0) |
| Vascular stenosis | 7 (10.6) |
| Vascular stenosis with need for intervention | 6 (9.1) |
| Vascular dissection | 2 (3.0) |
| Vascular dissection with need for intervention | 1 (1.5) |
| Treatment of vascular occlusion, stenosis or dissection after bailout MANTA | |
| Only endovascular ballooning | 5 (7.6) |
| Stent implantation | 3 (4.5) |
| Surgical repair | 1 (1.5) |
| Values are expressed as n (%). | |
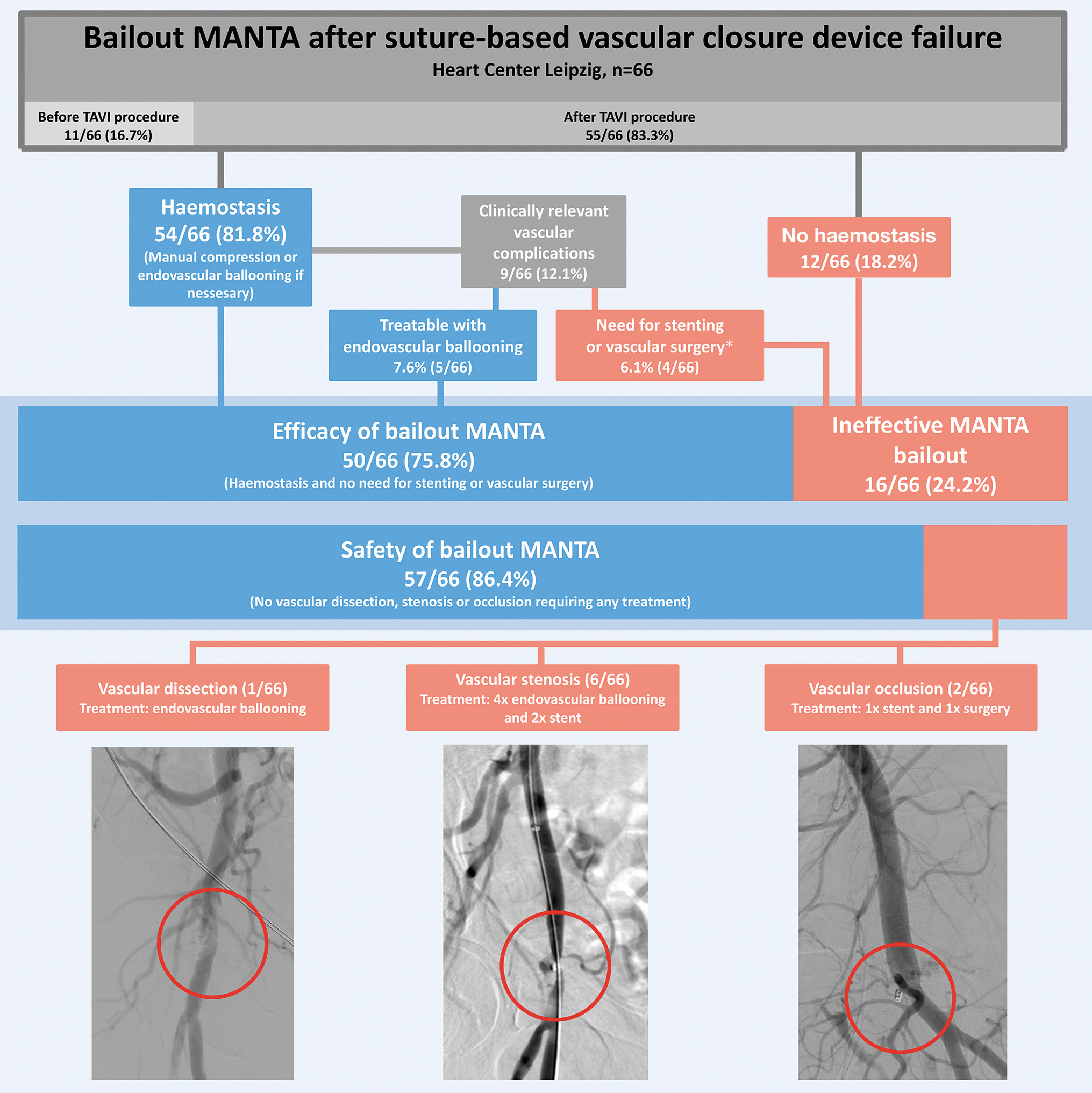
Central illustration. Efficacy and safety of bailout MANTA. *Treatment: stenting – 3 patients, surgical vascular repair – 1 patient. TAVI: transcatheter aortic valve implantation
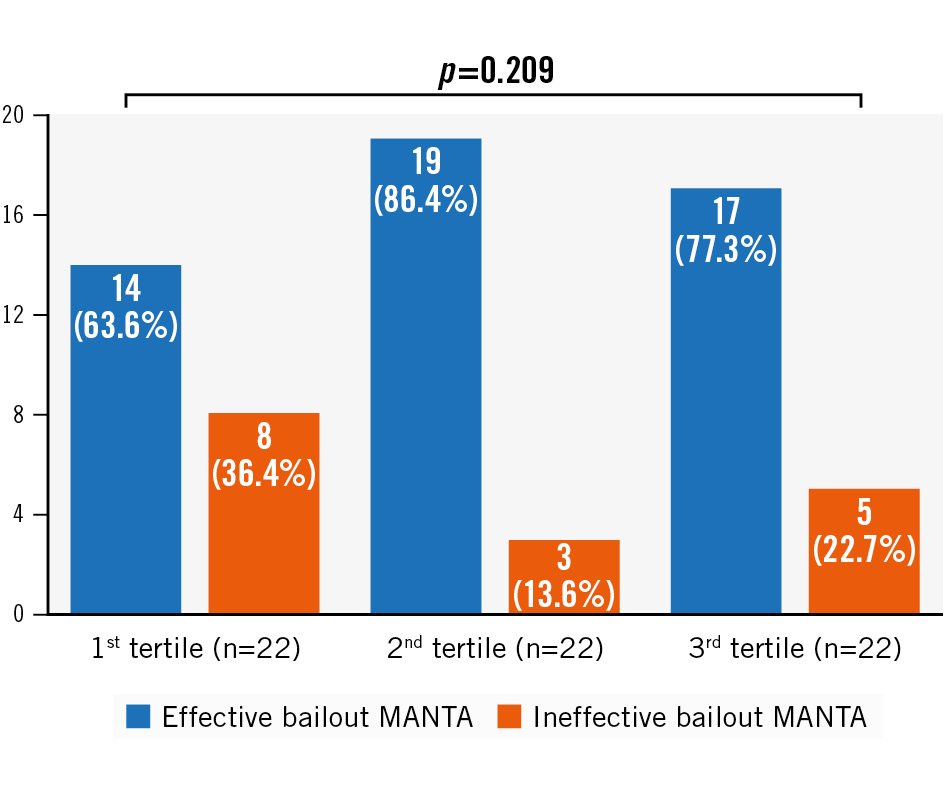
Figure 2. Efficacy of bailout MANTA according to tertiles of patient enrolment.
EFFICACY AND SAFETY OF BAILOUT VERSUS ELECTIVE MANTA PROCEDURES
A total of 258 patients were enrolled in the MANTA cohort of the CHOICE-CLOSURE trial at three centres in Germany, between June 2020 and June 2021. The baseline characteristics of elective (CHOICE-CLOSURE) and bailout MANTA patients were largely comparable. However, patients with a bailout MANTA procedure were more likely to have diabetes mellitus (56.1% vs 38.0%; p=0.012), a history of cerebrovascular disease (22.7% vs 10.1%; p=0.011) or severe renal insufficiency (18.2% vs 9.7%; p=0.025) (Supplementary Table 4). In addition, severe vascular calcification of the access site was more common in the bailout MANTA group (31.8% vs 12.7%; p≤0.001) (Supplementary Table 5). Only the 18 Fr MANTA VCD was used in the CHOICE-CLOSURE trial, while the 14 Fr VCD was used in 25.8% of patients in the bailout population (Supplementary Table 6).
The efficacy endpoint was achieved in 93.4% (241/258) and the safety endpoint in 94.6% (244/258) of elective MANTA patients. In comparison, the rates of both efficacy (75.8% vs 93.4%; p≤0.001) and safety (86.4% vs 94.6%; p=0.040) were significantly lower in the bailout MANTA population.
PREDICTORS OF EFFICACY
Most baseline characteristics were largely comparable between patients with and without an effective bailout MANTA application (Supplementary Table 7). However, differences were observed in terms of vascular characteristics. Patients with a successful bailout procedure had calcification of the access site that was more severe, numerically, (Supplementary Table 8), and anterior calcification was present significantly more often (56.0% vs 12.5%; p=0.003). Procedural characteristics were predominantly similar (Table 3). All patients received either a reduced dose or a full dose of protamine at the end of the procedure, with no difference in the efficacy endpoint between the two groups. Operators with more experience in applying the bailout MANTA technique were more likely to achieve effective haemostasis. In addition, patients with an effective bailout MANTA were less likely to have had a previously attempted vascular closure with more than two suture-based VCDs (4.0% vs 25.0%; p=0.027).
In multivariable analysis, operator experience (adjusted odds ratio [OR] 12.29, 95% confidence interval [CI]: 1.99-75.99; p=0.007) was the only independent predictor of an effective bailout MANTA procedure (Table 4). Conversely, the prior application of three ProGlide VCDs was associated with a reduced efficacy of the bailout MANTA technique (OR 0.02, 95% CI: <0.01-0.39; p=0.010).
Table 3. Procedural details stratified by the effectiveness of bailout MANTA.
| Variable | Effective bailout MANTA N=50 (75.8) |
Ineffective bailout MANTA N=16 (24.2) |
p-value |
|---|---|---|---|
| Main access site, right | 44/50 (88.0) | 15/16 (93.8) | 1.000 |
| Mean sheath size, Fr | 14 (14-16) | 14 (14-16) | 0.189 |
| Sheath-to-femoral artery ratio | 0.74 (0.66-0.88) | 0.75 (0.66-0.87) | 0.838 |
| Ultrasound-guided puncture | 15/50 (30.0) | 1/16 (6.25) | 0.091 |
| Number of ProGlides used | 0.017 | ||
| One | 14/50 (24.0) | 6/16 (37.5) | 0.166 |
| Two | 34/50 (54.0) | 6/16 (37.5) | 0.060 |
| Three | 2/50 (4.0) | 4/16 (25.0) | 0.027 |
| Heparin dose, IU | 10,000 (10,000-13,000) | 10,500 (9,500-13,500) | 0.912 |
| ACT at closure, sec | 147 (136-171) | 151 (137-159) | 0.883 |
| Use of protamine | 0.221 | ||
| None | 0/49 (0) | 0/16 (0) | |
| Less than full dose | 22/49 (44.9) | 10/16 (62.5) | |
| Full dose | 27/49 (55.1) | 6/16 (37.5) | |
| Fluoroscopy time, min | 16.3±8.1 | 32.7±25.8 | 0.001 |
| Contrast dye amount, ml | 94.8±32.7 | 159.2±70.5 | 0.001 |
| MANTA size | 0.205 | ||
| 14 Fr | 15/50 (30.0) | 2/16 (12.5) | |
| 18 Fr | 35/50 (70.0) | 14/16 (87.5) | |
| Experienced operator (≥10 bailout procedures) | 44/50 (88.0) | 9/16 (56.3) | 0.005 |
| Values are expressed as mean±SD, median (interquartile range) or n/N (%). ACT: activated clotting time; Fr: French; SD: standard deviation | |||
Table 4. Univariable and multivariable analysis of efficacy of bailout MANTA.
| Predictors | Univariable | Multivariable | ||||
|---|---|---|---|---|---|---|
| OR | 95% CI | p-value | adjusted OR | 95% CI | p-value | |
| Age | 0.92 | 0.83-1.02 | 0.123 | - | - | - |
| Sex, female | 0.34 | 0.11-1.10 | 0.068 | - | - | - |
| Body mass index | 0.98 | 0.89-1.09 | 0.745 | - | - | - |
| Diabetes | 0.72 | 0.23-2.24 | 0.575 | - | - | - |
| Peripheral arterial disease | 0.77 | 0.08-7.40 | 0.818 | - | - | - |
| Baseline platelet count, 109/l | 1.00 | 1.99-1.00 | 0.359 | - | - | - |
| Oral anticoagulation | 0.85 | 0.28-2.63 | 0.780 | - | - | - |
| Antiplatelet therapy | 1.31 | 0.41-4.16 | 0.648 | - | - | - |
| Severe vascular calcification at access site | 10.00 | 1.22-81.81 | 0.032 | 3.54 | 0.13-100.34 | 0.458 |
| Anterior vascular classification at access site | 8.91 | 1.83-43.40 | 0.007 | 10.71 | 0.58-198.38 | 0.111 |
| Prior use of three ProGlides | 0.13 | 0.02-0.77 | 0.024 | 0.02 | <0.01-0.39 | 0.010 |
| Common femoral artery diameter | 0.98 | 0.69-1.39 | 0.887 | - | - | - |
| Mean sheath size, French | 0.75 | 0.47-1.20 | 0.225 | - | - | - |
| Sheath-to-femoral artery ratio | 1.21 | 0.07-20.54 | 0.897 | - | - | - |
| 14 French MANTA | 3.00 | 0.61-14.68 | 0.178 | - | - | - |
| Ultrasound-guided puncture | 6.43 | 0.78-53.17 | 0.084 | - | - | - |
| Experienced operator (≥10 bailout procedures) | 5.70 | 1.55-21.04 | 0.009 | 12.29 | 1.99-75.99 | 0.007 |
| CI: confidence interval; OR: odds ratio | ||||||
BAILOUT MANTA FAILURE MODES
Patients with bailout failure more commonly had failed haemostasis (12/16) than vascular occlusion requiring stent implantation or surgical repair (4/16). A typical failure mechanism was observed in each of these groups. If bleeding persisted, the MANTA VCD had been implanted too superficially (Figure 3). In patients with severe vascular stenosis or occlusion, the MANTA VCD had been applied too deeply into the vessel and had led to stenosis due to displaced vascular calcification or a suboptimal toggle position (Central illustration).
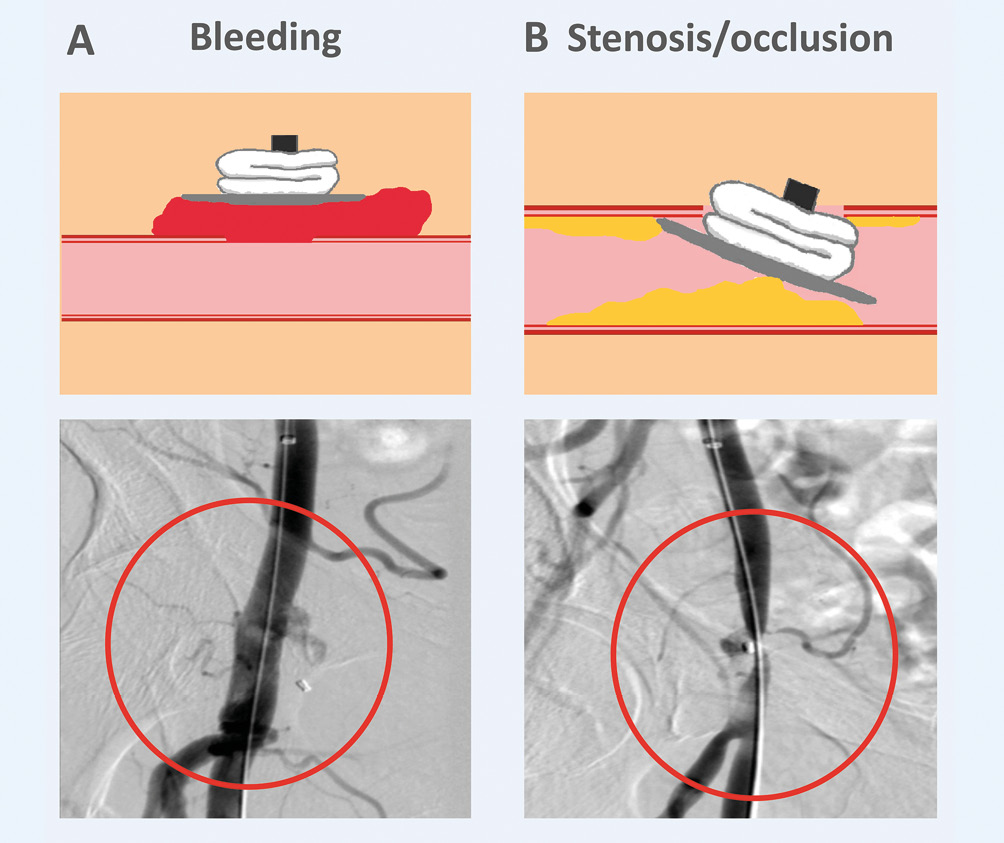
Figure 3. Failure modes of bailout MANTA. A) Inadvertent superficial application of the MANTA device resulting in persistent bleeding. B) Deep, partially intravascular, application resulting in stenosis or occlusion.
Discussion
To the best of our knowledge, this is the first systematic study analysing the bailout MANTA technique following the failure of suture-based vascular closure in patients undergoing transfemoral TAVI. The main findings of the study are as follows: 1) bailout MANTA is safe and effective in a large proportion of patients with upstream or downstream suture-based VCD failure; and 2) operator experience appears to be a crucial aspect with the current-generation device.
The baseline characteristics of this study cohort reflect a population with difficult vascular access. Known risk factors for VCD failure, such as moderate or severe vascular calcification or tortuosity, were predominant16. In addition, nearly half of the patients had anterior wall calcification, and patients were commonly overweight17. Overall, the results of this study suggest bailout MANTA as an additional step in the escalation algorithm in case of suture-based VCD failure. If two suture-based VCDs do not significantly reduce bleeding, bailout MANTA can be applied as the next step. Supportive manual compression and/or endovascular ballooning should subsequently be applied if necessary.
We could not demonstrate a significant learning curve with the bailout technique at the institutional level in this study. This can be attributed both to the overall limited number of cases and to the relatively large number of interventionalists with individual learning curves during the study period. However, individual operator experience was an essential factor in the success of the bailout attempt. Since previously published data on elective MANTA application have not indicated a relevant learning curve18, it appears that tackling the previously mentioned challenges of depth measurement and correct application of the plug during a bailout situation requires experience. Therefore, it is not surprising that both efficacy and safety were achieved less frequently with bailout MANTA compared to the elective MANTA cohort of the CHOICE-CLOSURE trial. As already described, the downstream measurement of implantation depth is more challenging with bailout MANTA, and the technique is more demanding.
Therefore, optimisation of depth measurement could further improve the efficacy of the MANTA bailout technique and, in particular, reduce the proportion of inadvertent superficial implantations, which can potentially be reduced if depth measurement becomes as accurate as in the elective setting. A first step could be the implementation of the previously mentioned adapted technique. The MANTA depth measurement should be adjusted by measuring the implantation depth under slight compression of the surrounding tissue and adding two centimetres instead of one centimetre to the measured puncture depth. Second, a larger depth locator of 14 Fr could allow more accurate measurements without manual compression by completely sealing the puncture site. Such a device has recently been launched but was not available during the study period. A further possibility could be the use of ultrasound to guide accurate application in the target vessel, which has been demonstrated by Moriyama et al in the elective setting19. Finally, inflating a balloon during deployment may be useful as it would stop bleeding and may facilitate MANTA depth measurement as well as implantation. However, we do not have experience with the routine use of endovascular ballooning during bailout MANTA, and further studies are needed to determine if such an approach may further enhance efficacy.
Prior use of three ProGlides was a further predictor associated with a less frequent occurrence of the efficacy endpoint. While we cannot provide a definite explanation for this association, it can be assumed that the need for three suture-based VCDs indicates an extreme form of VCD failure, making a bailout MANTA application more difficult because of severe bleeding. It is also possible that effective haemostasis in such cases may no longer be possible with MANTA due to repeated vascular manipulation and the potential expansion of arterial injury. This observation may suggest that bailout MANTA should be considered at an early stage of suture-based VCD failure. However, this study only includes 6 cases of bailout MANTA after the failure of three ProGlides, which significantly limits the observed statistical association.
Interestingly, vascular complications associated with the MANTA bailout attempt seem to be treatable in the majority of patients with endovascular ballooning. However, stent implantation is still a possible option if the MANTA bailout attempt fails.
Whether the bailout MANTA technique is superior to direct stenting remains unknown. Overall, stent implantation after VCD failure seems to be associated with a low complication rate during follow-up20. Nevertheless, several aspects support a primary bailout MANTA attempt. First, the application of a MANTA VCD is faster and easier than stenting the vascular access site. Second, in recent years, the TAVI population has become increasingly younger, and considerations of a future valve-in-valve procedure are of increasing importance21. In this context, stented iliofemoral vessels may be a significant limitation for subsequent procedures. Finally, a successful bailout MANTA can avoid more aggressive antithrombotic therapy due to stent implantation.
The randomised CHOICE-CLOSURE and MASH trials found no advantage of a systematic use of the MANTA VCD compared with the ProGlide VCD after TAVI56, and MANTA was even associated with a higher rate of access site-related vascular complications in the CHOICE-CLOSURE trial6. Nevertheless, its efficacy as a bailout device appears to justify its presence among the toolbox of devices needed for contemporary percutaneous interventions requiring large-bore arterial access.
Limitations
This study has some important limitations. First, this is a non-randomised study and the choice of the bailout technique was made by the interventionalist. Thus, selection bias cannot be excluded. Second, because of the heterogeneous patient population and the small number of included patients, a direct comparison between the bailout MANTA technique and covered stent implantation was not performed. Third, the results may not be generalisable due to the monocentric study design and the high volume and experience of the study centre. Finally, the indication for using MANTA as a bailout device was not standardised. Therefore, it remains unclear whether the use of different additional closure devices would have been sufficient for haemostasis in some of the included cases.
Conclusions
Bailout application of the large-bore plug-based MANTA device was effective and safe in the majority of patients with suture-based VCD failure during transfemoral TAVI. Operator experience seems to be a crucial aspect with the current-generation device, which was not designed for bailout application. Further technological refinements to facilitate accurate placement in a bailout setting appear to be necessary.
Impact on daily practice
There are limited options for suture-based vascular closure device (VCD) failure after transfemoral TAVI. Anecdotally, the plug-based MANTA VCD has been suggested as a bailout device. Bailout MANTA after suture-based VCD failure was effective and safe in this study, but operator experience seems to be crucial with the current-generation device.
Acknowledgements
We would like to thank all CHOICE-CLOSURE investigators for their support and contribution of patient-level data. Furthermore, we thank Mrs Salome Hecht for her significant contribution to data collection.
Funding
There was no external funding source for this study.
Conflict of interest statement
M. Abdel-Wahab reports that his hospital receives speaker honoraria and/or consultancy fees on his behalf from Boston Scientific, Abbott, and Medtronic. The other authors have no conflicts of interest to declare.
Supplementary data
To read the full content of this article, please download the PDF.

