The term TAVI is currently part of familiar language. But who invented this acronym? Let’s go back to the beginning of catheter-based interventions (Figure 1).
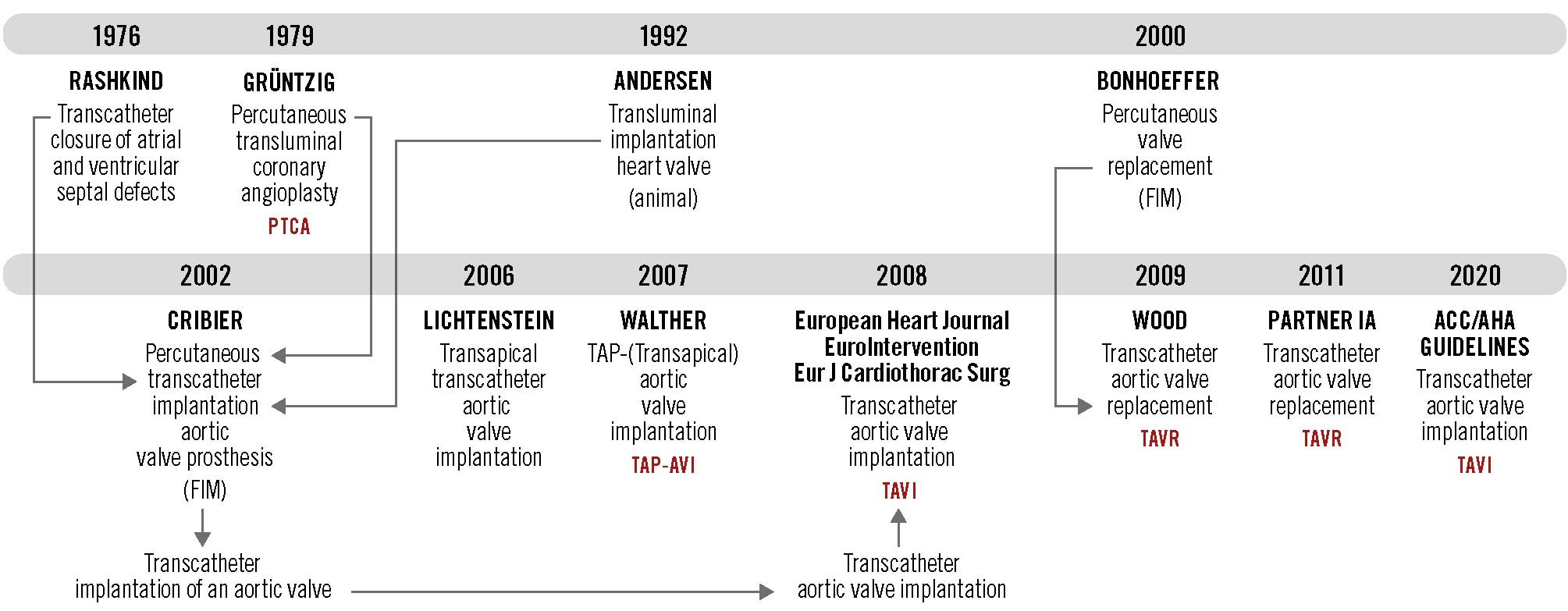
Figure 1. The history of the acronym TAVI. FIM: first-in-man
Where does the term “TAVI” come from?
In 1979, Andreas Grüntzig presented the results of non-operative dilatation of coronary artery stenosis. He used the acronym PTCA which incorporated the words employed by his famous predecessors, in chronological order: “percutaneous” (Seldinger), “transluminal” (Dotter), “coronary” (Judkins) and “angioplasty” (Zeitler).
In 1992, Henning Andersen reported his results with a new expandable aortic valve in closed-chest pigs, using the terms “implantation”, “artificial heart valve” and “transluminal”1. He was inspired by Julio Palmaz, whom he heard at a conference in Scottsdale, Arizona, USA in 1989. By an amazing coincidence, Julio had the idea of a balloon-expandable stent whilst attending a conference by Andreas Grüntzig in New Orleans, Louisiana, USA, eleven years earlier, in 1978. But Henning Andersen was mistaken when he said that Charles Dotter had conducted a lecture on angioplasty in Frankfurt, Germany in 1964 which had been attended by Andreas Grüntzig. That particular year, Charles Dotter had been in Portland, Oregon, USA, and Andreas Grüntzig was obtaining his medical degree from the University of Heidelberg, Germany. In fact, the lecture referred to by Andersen was given by Eberhard Zeitler – who contributed to the development of Dotter’s method in Europe – 5 years later, in 1969, just before Andreas arrived in Zurich, Switzerland.
In 2000, Philipp Bonhoeffer reported the first-in-man (FIM) stent implantation combined with a valve replacement in a right ventricle to pulmonary artery prosthetic conduit with valve dysfunction2. He used the terms “replacement”, “valve” and “percutaneous”. The terms “percutaneous” and “transluminal” were used by Andreas Grüntzig in 1979.
In 2002, Alain Cribier reported the FIM non-operative treatment of calcific aortic stenosis3, using the terms “percutaneous” and “transcatheter implantation of an aortic valve”. The term “transcatheter” was originally used for therapeutic arterial embolisations in the early 1970s and for the first time in the field of cardiology in 1976, when William Rashkind related his experience with transcatheter closure of atrial and ventricular septal defects in experimental animals. This word was adopted in 1989 for the TCT (Transcatheter Cardiovascular Therapeutics) meeting launched by Kenneth Kent, Martin Leon, Augusto Pichard and Lowell Satler. Alain initially used the acronym PHV (percutaneous heart valve).
In 2006, the transapical approach induced a radical shift, and Samuel Lichtenstein thereafter spoke of transapical transcatheter aortic valve implantation. In 2007, the acronym TAP-AVI for “transapical aortic valve implantation” was proposed by Thomas Walther4. The term “percutaneous” disappears in favour of “transcatheter”. Alain Cribier also transformed the acronym PHV to THV (transcatheter heart valve).
In 2008, a position statement from the European Association of Cardio-Thoracic Surgery (EACTS) and the European Society of Cardiology (ESC), in collaboration with the European Association of Percutaneous Cardiovascular Interventions (EAPCI), concerning transcatheter valve implantation for patients with aortic stenosis, was published in 3 journals under the leadership of Alec Vahanian. The position statement was published in the European Heart Journal in June, in the European Journal of Cardio-Thoracic Surgery in July and in EuroIntervention in August5. The acronym TAVI for “transcatheter aortic valve implantation” appeared for the first time in these joint publications. It was in fact a revival of the terms initially used by Alain Cribier in 2002, removing the term “percutaneous” and changing the expression “implantation of an aortic valve” to “aortic valve implantation”, which is more consistent with the English language. In fact, TAVI sounds better than TIAV... and, coincidentally, TAVI in French, phonetically, means “your life”â... Without knowing it, Alain Cribier was indirectly but likely responsible for the origin of the acronym TAVI.
But the story doesn’t end here...
TAVI or TAVR? How to choose?
In 2007, the term TAVR appeared with the CoreValve TAVR ReValving clinical trial, whereby Rüdiger Lange related the first successful transapical aortic valve implantation with the CoreValve Revalving System (Medtronic). The following year, Hendrik Ruge reported the first successful aortic valve implantation with the CoreValve Revalving System via right subclavian artery access. In this case, the transapical delivery system was not available at the time of surgery. In both these cases, the letter T stood for “transapical”.
In 2009, the acronym TAVR for “transcatheter aortic valve replacement” appeared for the first time6. Transcatheter included both surgical and percutaneous approaches.
In 2010, Martin Leon still used the acronym TAVI in The Placement of AoRtic TraNscathetER Valves (PARTNER IB) Trial using the Edwards SAPIEN heart-valve system (Edwards Lifesciences): Transcatheter Aortic-Valve Implantation for Aortic Stenosis in Patients Who Cannot Undergo Surgery.
In 2011, however, the term “replacement” was used in preference to “implantation” in the PARTNER IA trial: Transcatheter versus Surgical Aortic-Valve Replacement in High-risk Patients. The main reason for this was to get easier U.S. Food and Drug Administration (FDA) approval. Furthermore, reimbursement for TAVI required a similar code to surgery: transcatheter AVR may well be compared with surgical AVR. TAVR was subsequently used in the PARTNER 2 Trial (Transcatheter or Surgical Aortic-Valve Replacement in Intermediate-Risk Patients) and the PARTNER 3 Trial (Transcatheter Aortic-Valve Replacement with a Balloon-Expandable Valve in Low-Risk Patients).
Finally, in an effort to homogenise the acronyms, in the latest 2020 ACC/AHA Guideline for the Management of Patients with Valvular Heart Disease, the acronym TAVI has been reintroduced in place of TAVR7. The right choice?
Conflict of interest statement
The author has no conflicts of interest to declare.

