In 2012, I wrote an abstract that was never accepted by any national or international congress. I would like to reproduce it here:
“Background: Professor Patrick W. Serruys (PWS) has been the Chief of the Interventional Cardiology Department at the Thoraxcenter, Rotterdam. The Thoraxcenter has been the leading centre in Europe in the field of stenting and many fellows were eager to be accepted for training by the Professor. The aim of this study was to determine the influence of PWS on the outcomes of a fellow arriving from a southern European country.
Methods: This is a single-centre, single-arm, non-randomised, prospective and totally uncontrolled study. Neither the Ethics Committee of the centre nor the fellow had any idea about the trial. In 1997, a single fellow (“patient”) was included in the trial. The patient signed an informed consent in order to attend evening meetings during the weekends at PWS’ home. The patient was trained for two years and has been followed up for 20 additional years.
Results: During his training, the patient was able to perform many coronary procedures involving stenting, IVUS, FFR and intracoronary brachytherapy. Specifically, the patient became an expert in cleaning the guidewires for PWS during the night shifts. During his stay in Rotterdam, the patient performed a number of QCA and 3D longitudinal IVUS analyses, making the weekends peaceful and relaxed. Besides, the fellow could always call his pregnant wife on a daily basis and, as such, could arrive in time (the day before) for the delivery of his first daughter. From the research point of view, he could write and correct many papers, rewrite and correct again, rewrite and correct again… Interestingly, all of them were finally accepted! He could then defend his PhD thesis that was awarded cum laude. A multivariate analysis was performed to identify the predictors of survival (in Rotterdam). After adjusting for other confounders such as weather conditions (always raining), nice friendship with other fellows, and safe trips with Jurgen Ligthart in his Model A Ford, PWS remained as the only independent predictor of success (OR: 25.7; 95% CI: 5.0-37.3; p<0.0001). After Rotterdam withdrawal, no fellow thrombosis occurred. He went back first to Madrid and later to Barcelona. He is currently the Chief of the Interventional Cardiology Department at the Clinic Hospital in Barcelona. He is now happy, mentally stable and has extraordinary memories of PWS playing tennis. At 20-year follow-up he is still alive without the occurrence of any major adverse psychiatric events.
Conclusions: This single-patient trial demonstrated without any doubt (Class of recommendation I, level of evidence A) that PWS had decisive influence on the outcomes of the fellow, namely Manel Sabaté. Many other trials have been performed over the last 30 years corroborating these results. A meta-analysis of all trials is currently ongoing”.
As a matter of fact, this abstract was fondly prepared as a tribute to Professor Patrick Serruys’ 30-year career at the Thoraxcenter (Rotterdam, the Netherlands; May 19, 2012).
The relationship between a fellow and his/her senior may become something special. To some extent, it may mimic the use of the “mother-and-child” technique1 that usually provides the required support to deliver the device to the desired location. Similarly, a fellow-in-training (Figure 1A, Figure 1B) needs support and self-confidence but also supervision and advice under certain circumstances. On the one hand, the senior should give support and be mentor to the fellow. He or she should be a model for the fellow - someone to be mirrored. Besides, the senior has to make the fellow react and change procedural behaviour in order to improve his/her skills. The experience of the senior should be transferred to the fellow by doing rather than by saying. One may find the theory in books2,3, test devices in simulators and see live cases in dedicated courses. However, the art of learning by doing can only be performed in the catheterisation laboratory in front of the patient and under the supervision of the senior. In my view, the senior has to suggest rather than to impose a strategy, as many procedures can be properly performed in different ways. Ideally, procedures should be discussed upfront among the senior, the fellow and the rest of the team and be well prepared for eventual complications.
Figure 1. Image of a fellow in training. A) Warning signal of a fellow in training. B) Professor Patrick Serruys with his fellow Manel Sabaté after performing a procedure in 1998.
On the other hand, the fellow has to be realistic about his/her limitations. At the beginning, it is not unusual to feel dumb when you are unable to perform a selective catheterisation for 15 minutes and four different catheters and the senior with your initial catheter successfully cannulates the coronary artery in two seconds. Then, you ask with resignation, how did you do that? It is just a matter of experience. The fellow is not supposed to be able to perform perfect procedures from the very beginning, but his/her work has to inspire confidence with the senior and the rest of the team. The fellow has to listen and be receptive to advice from the most experienced personnel (including other staff, nurses and technicians) and put them into practice. Sharing experiences with other colleagues by the use of current social media is also another way to increase your experience. Overall, the fellow has to be open-minded, perseverant, respectful, meticulous, humble, and self-critical. The fellow has to assume that, at the end of the day, the senior has the final responsibility for the right care of the patient and clinical decisions (including the role of the fellow in the procedure) should be based on this perspective.
Do not forget that your fellows will be your legacy (Figure 2). If one looks at the genealogical tree of the mentor with all the fellows who have been taught during his/her career, one may be able to quantify how his/her teaching has influenced the world. The fellow of today will be the senior of tomorrow (Figure 3). As in The Lion King, “it is the circle of life and it moves us all, through despair and hope, through faith and love, till we find our place, on the path unwinding”4.

Figure 2. Rotterdam, the Netherlands, 19 May 2012. Professor Patrick Serruys with most of his fellows, his family, relatives and friends.
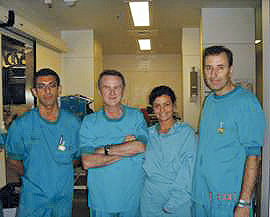
Figure 3. Professor Colombo with the “senior” Manel Sabaté and two fellows-in-training, Salvatore Brugaletta and Clarissa Cola, in 2008 after performing the first TAVI procedure at Sant Pau Hospital, Barcelona.
Conflict of interest statement
M. Sabaté was fellow at the Thoraxcenter between 1997 and 1999.

